Adult Traumatic Agonal Arrest and Resuscitation
Purpose
To outline the procedure for the treatment of the adult traumatic patient with a penetrating or blunt mechanism of injury who has no signs of life.
In patients without signs of life for >10 minutes in blunt trauma or >15 minutes in penetrating trauma, it is appropriate to terminate resuscitation efforts. Trauma surgeon discretion required as reported pre hospital CPR times may be inaccurate.
Definitions
- Blunt trauma –physical impact to the body by some force
- Penetrating trauma - occurs when a foreign object pierces the skin and enters the body creating a wound
- Adult trauma patient – any patient age fifteen (15) years or older who has sustained a blunt injury
- Agonal arrest - a severely injured patient in extremis, with no signs of life (absent pulse, absent respirations, absent pupil response, GCS 3)
Background
- Resuscitation of the adult trauma patient who is agonal or arrests as a result of a penetrating or blunt mechanism consist of a rapid assessment and treatment of the various measures of PEA (profound hypovolemia, airway compromise, tension pneumothorax and pericardial tamponade).
- Drowning, lightning strikes, medical causes of cardiac arrest, patients with profound hypothermia or if the patient’s age is 14 years and less are excluded from this guideline.
- The utilization of Advanced Cardiac Life Support (ACLS) and Basic Life Support (BLS) measures, including use of the Lucas device, in the setting of Advance Trauma Life Support (ATLS) resuscitation is of limited, if any, benefit in the setting of blunt traumatic patient arrest.
- Consider previous establishment of the patient’s DNR/DNI status, especially in patients who reside in a long term health care facility.
- Procedures (including airway assessment, chest tubes, etc.) take priority over chest compressions in the trauma patient in agonal or arrest states.
Resuscitation Algorithm
CONSIDER removal of Lucas device/mechanical chest compression device upon patient’s arrival in trauma bay.
- Airway:
-
- Non-intubated patient
-
- Obtain adequate airway (definitive ideal, however, if King, LMA or iGel is adequate, continue until pt stabilizes)
-
- Confirmation of Airway placement
-
- Visualization of ETT placement through vocal cords, if applicable
- Colorimetric CO2 detector (may not be reliable in arrest)
- Auscultation of bilateral breath sounds; absence of delivered breath sounds over epigastrium
- Appropriate O2 Saturation
-
- Intubated Patient
-
- Clear communication of assessment to trauma leader
- Confirmation of airway placement by ER faculty at head of bed
- Colorimetric CO2 detector (may not be reliable in arrest)
- Direct laryngoscopy may be considered in setting of any question of placement of ETT. Direct laryngoscopy in presence of ETT has a risk of dislodgement of appropriately placed ETT.
- Auscultation of bilateral breath sounds; absence of delivered breath sounds over epigastrium
- Appropriate O2 saturation
-
- Non-intubated patient
-
- Breathing:
-
- Bilateral Chest Tube Thoracostomy
- Resuscitative Thoracotomy (see Western Trauma algorithm below)
-
- Circulation:
-
- Rapid assessment of central (femoral) and peripheral pulses (radial, pedal)
- Clear communication of assessment to trauma leader
- Control of life-threatening external hemorrhage (hold pressure, tourniquet, etc)
- Obtain manual blood pressure (will not be present if no pulse)
- Confirmation of in-place intravenous (IV) access
- If no IV access:
-
- Establish IV, Intraosseous (IO) or central access
- Rapid, early delivery of Whole blood or Packed Red Blood Cells/plasma
-
- Consider initiation of Massive Blood Transfusion (MBT) protocol
- Maintain 1:1:1 ratios
-
-
- Attach cardiac leads/monitor
- Check Cardiac window on Focused Assessment with Sonography in Trauma (FAST)
-
- Assess for pericardial effusion
- Assess cardiac kinetic activity
-
-
- Disability:
-
- Glasgow Coma Scale (GCS) measurement
- Pupillary response
-
- Exposure/Environment
-
- Rapid and complete patient exposure
- Rapidly cover the exposed patient with warmed blankets (allow above assessment and procedures)
- Ensure underbody Bair Hugger functional (or provide warmth by another means)
-
During ABCDEs in a blunt agonal arrest, determine length of time of CPR and quickly assess patient for signs of life (detectable blood pressure, respiratory or motor effort, cardiac electrical activity, or pupillary activity)
- If CPR<10 min in blunt trauma or <15 minutes in penetrating trauma, AND pt has signs of life, proceed with Resuscitative Thoracotomy (see Western Trauma Association algorithm below).
- If CPR>10 min in blunt trauma or <15 minutes in penetrating trauma, AND NO signs of life, pt should be pronounced dead.
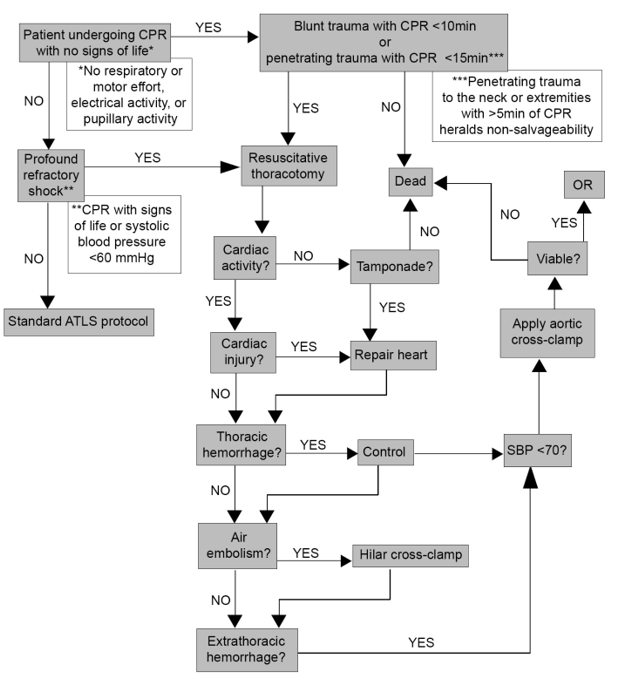
FIGURE 1. Western Trauma Resuscitative Thoracotomy algorithm
https://www.westerntrauma.org/wp-content/uploads/2020/08/Resuscitative-Thoracotomy_FINAL.svg
References
- Trauma patients receiving CPR: Predictors of Survival. J Trauma 2005 58:951-958. Pickens JJ, Copass MK, Bulger EM.
- Blunt Trauma Patients with Prehospital Pulseless Electrical Activity (PEA): Poor Ending Assured. J Trauma 2002 53:876-881. Martin SK, Shatney CH, Sherck JP, Ho C, Homan SJ, Neff J.
- Confusion Surrounding the Treatment of Traumatic Cardiac Arrest. Journal of the American College of Surgeons. Fulton RL, Voigt WJ, Hilakos AS.
- Role of External Cardiac Compression in Truncal Trauma. J Trauma 1982 Vol. 22 No.11. Mattox KL, Feliciano DV.
- Hemodynamic Effects of External Cardiac Massage in Trauma Shock. J Trauma 1989 Vol. 29 No. 10. Luna GK, Pavilin EG, Kirkman T, Copass MK, Rice CL.
- Guidelines for Withholding or Termination of Resuscitation In Prehospital Traumatic Cardiopulmonary Arrest: A Joint Position Paper From the National Association of EMS Physicians Standards and Clinical Practice Committee and the American College of Surgeons Committee on Trauma. Prehospital Emergency Care January / March 2003 Vol 7 / No. 1 141-146
- Withholding of Resuscitation for Adult Traumatic Cardiopulmonary Arrest: National Association of EMS Physicians and American College of Surgeons Committee on Trauma. Prehospital Emergency Care 2013 17:291
Authors
Charity Evans, MD | Division of Acute Care Surgery, Faculty | Principle Author
Last Updated
February, 2024