Evaluation and Management of Blunt Splenic Injury
Purpose
Splenic injury is one of the most common injuries following blunt abdominal trauma and can result in significant bleeding given the vascular nature of this organ. Unrecognized injury can be a cause of preventable death following trauma. The following guidelines outline the approach that should be taken when evaluating and managing a trauma patient with splenic injury and the decision-making process between operative and non-operative management.
Background/Definitions
During the last century, management of blunt splenic injury has shifted from observation/expectant management in the early 1900s to operative intervention for all injuries, to the current practice of selective operative and non-operative management of splenic injury. The current non-operative paradigm in adults was stimulated by the success of non-operative management of solid-organ injuries in hemodynamically stable children. The potential advantages of non-operative management include lower hospital cost, earlier discharge, avoiding nontherapeutic laparotomies (as well as associated cost and morbidity), fewer intra-abdominal complications, and reduced transfusion rates associated with an overall mortality of these injuries. While the non-operative approach to blunt splenic injury has been proven to work well in hemodynamically stable patients with lower grade injuries, there is still a role for operative and/or endovascular intervention in those patients who are hemodynamically unstable or those with higher grade injuries.
Splenic injuries are classified by a grading system established by the AAST (American Association for the Surgery of Trauma). In general, the higher the grade equals more severe injury and potential for associated morbidity and mortality.
AAST Splenic Injury Grading Scale
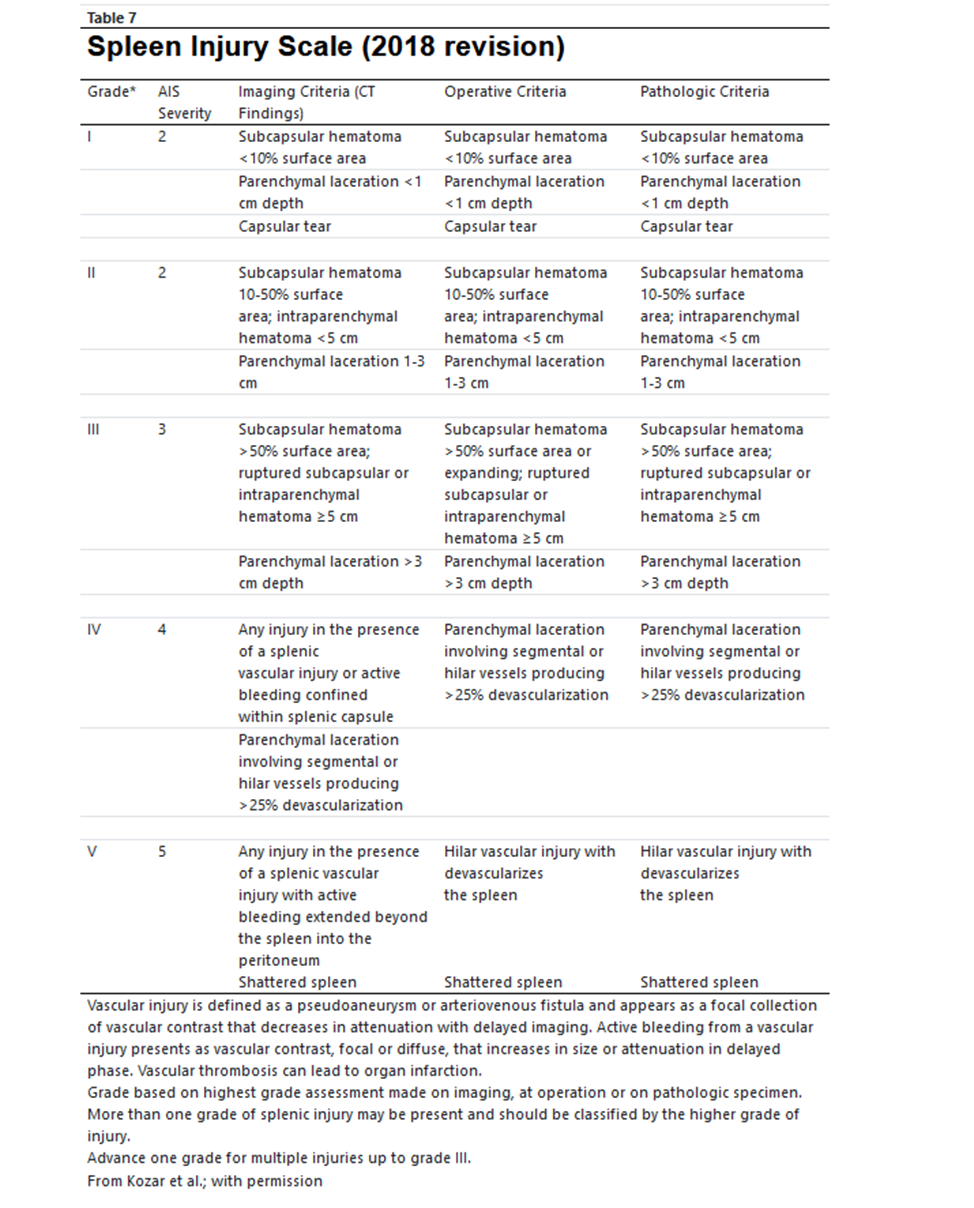
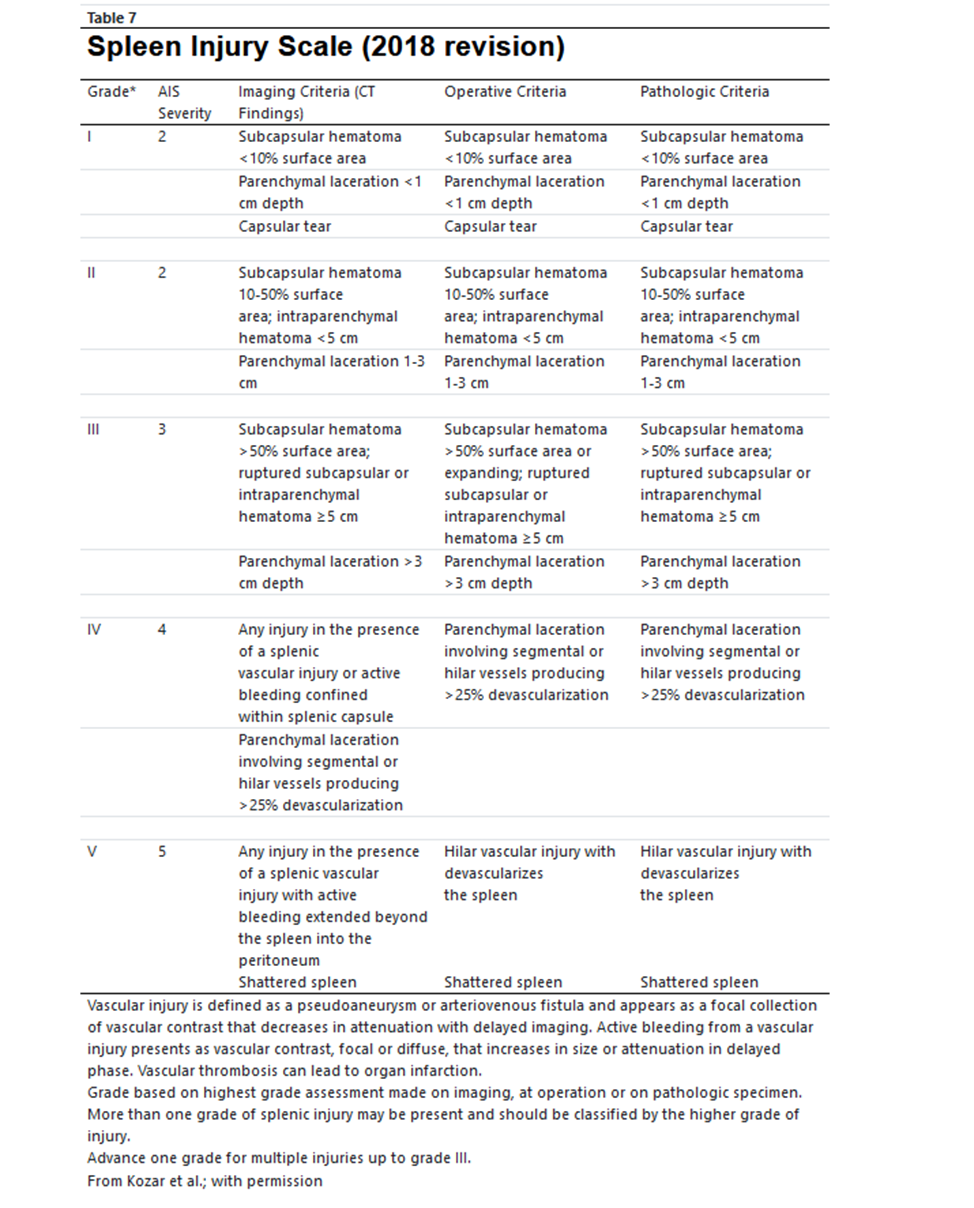
https://www.aast.org/resources-detail/injury-scoring-scale#spleen
Guideline Inclusion Criteria
- All trauma patients sustaining blunt abdominal trauma should be evaluated for potential splenic injury.
Guideline Exclusion Criteria
- Patients who no longer have a spleen.
- Pediatric patients <15 yrs age.
Diagnostic Evaluation
- All trauma patients should be initially evaluated per ATLS guidelines with work-up as mechanism and clinical presentation dictate.
- Resuscitative measures should be initiated as clinical status/presentation dictates.
- Labs, imaging and additional tests should be obtained as clinical status/presentation dictates.
- If a patient is hemodynamically UNSTABLE, minimal testing/imaging should occur prior to interventions for hemorrhage control.
Practice Recommendations for Management
- Once splenic injury is suspected and/or confirmed, management of that injury is dictated largely by the clinical status of the patient.
-
- If a patient is hemodynamically UNSTABLE:
-
- Initiate/continue resuscitative measures.
- Obtain an eFAST exam.
- If eFAST is positive, proceed to OR for surgical exploration.
-
- If a patient is hemodynamically STABLE:
-
- May continue with evaluation and work-up as mechanism and presentation dictate.
- Obtain imaging as indicated, including a multi-phase CT abd/pelvis with IV contrast
- Determine appropriate management strategy based on grade of injury, presence of blush/extravasation on imaging, and clinical status and injury burden of patient.
-
- If a patient is hemodynamically UNSTABLE:
-
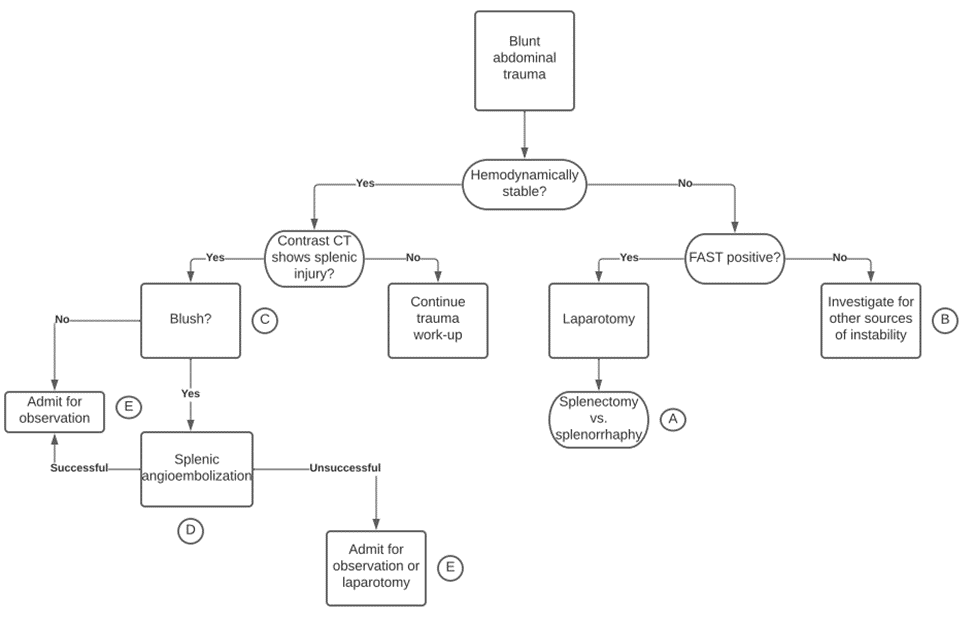
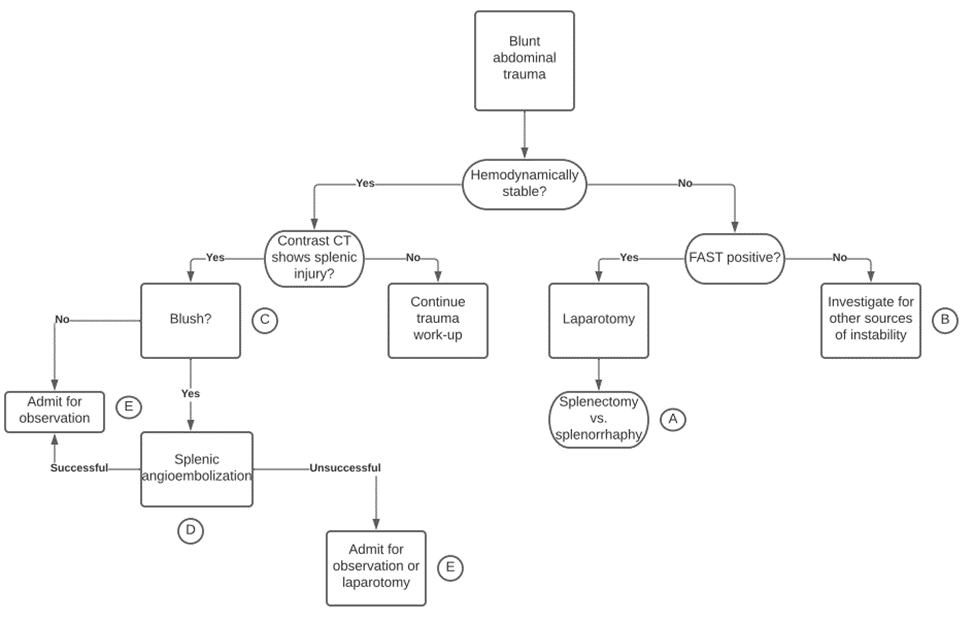
603730a847af494fa170694b778b703a.pdf (cvent.com)
- Operative Management
-
- Should be used in all patients who are hemodynamically unstable or those with peritonitis on exam.
- Should be considered in patients who are transient responders to resuscitation or in those with injury burden (head injury) in which hypotension secondary to hemorrhagic shock would be detrimental.
- Operative plan should be exploratory laparotomy for trauma with splenectomy vs splenorrhaphy.
-
- Splenic salvage/splenorrhaphy may be considered in Grade I-II injuries depending on the clinical status of the patient.
- Splenectomy should be performed in Grade III-V injuries or in patients with ongoing bleeding.
-
-
- IR Angioembolization
-
- Should be considered in patients who are transient responders to resuscitation, those with evidence of active extravasation/blush on CT abd/pelvis, those with high grade injuries (Grade III-V) or those with injury burden (e.g. head injury) in which hypotension secondary to hemorrhagic shock would be detrimental.
-
- Non-operative Management
-
- Non-operative management of splenic injuries should ONLY be considered in hemodynamically stable patients.
- Patients undergoing non-operative management should be monitored closely for deterioration in clinical status suggestive of ongoing hemorrhage (i.e. failure of non-operative management) with vitals per unit protocol, serial labs, abdominal exams and repeat imaging as indicated.
- Suggested non-operative management strategy is as follows:
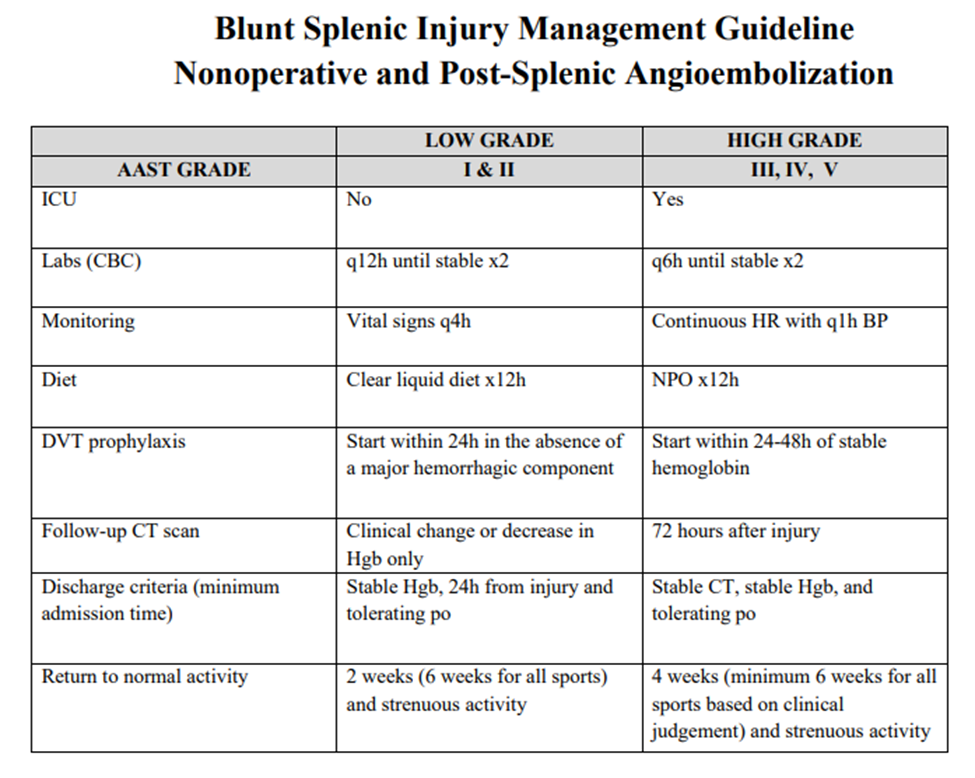
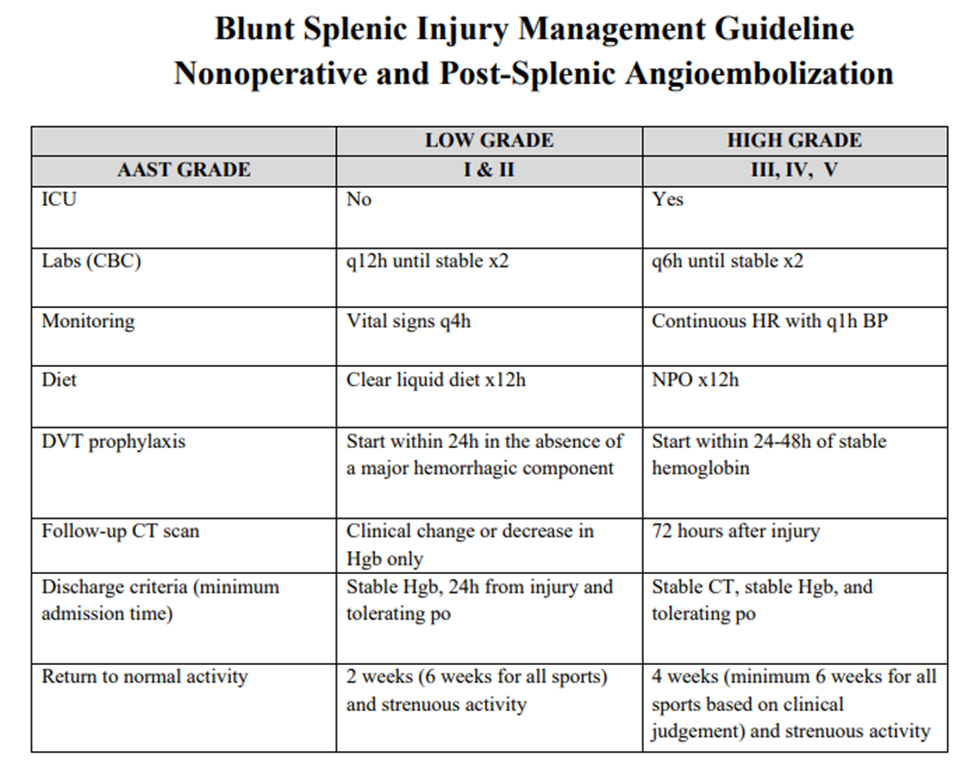
-
603730a847af494fa170694b778b703a.pdf (cvent.com)
-
-
- Repeat imaging for splenic injuries managed non-operatively
-
- A repeat multi-phase CT abd/pelvis with IV contrast should be obtained for all Grade III or higher splenic injuries between 3-5 days post injury or prior to discharge to evaluate for development of post-traumatic pseudoaneurysms.
- If pseudoaneurysms are present, then IR should be consulted for consideration of splenic angioembolization.
-
- Repeat imaging for splenic injuries managed non-operatively
-
- Follow-up Care:
-
- Post splenectomy vaccines
-
- Patients undergoing splenectomy as management of their splenic injury should obtain the following vaccines prior to discharge or at 14 days post-op (whichever date comes first)
-
- Quadravalent meningococcus (Menactra or Menomune)
- Pneumococcus (Pneumovax 23)
- H.influenzae B (HIB, ActHIB)
- Viral influenza vaccine (depending on time of year)
-
- Patients undergoing splenic angioembolization do not routinely require vaccinations.
- Patients undergoing splenectomy as management of their splenic injury should obtain the following vaccines prior to discharge or at 14 days post-op (whichever date comes first)
-
- All patients with splenic injury should follow-up in trauma clinic 1-2 weeks following discharge pending clinical status at time of discharge and hospital length of stay following injury.
- Post splenectomy vaccines
-
Outcome Measures and Guideline Adherence
- Time to OR/IR and interventions for all hemodynamically unstable patients will be tracked through our performance improvement process/initiatives.
- Patients failing non-operative management (i.e. those requiring IR angioembolization or exploratory laparotomy in a delayed fashion) will be tracked through our performance improvement process/initiatives.
- Adherence to obtaining repeat imaging for Grade III or higher splenic injuries at post-injury day 3-5 and need for subsequent interventions will be assessed every 6 months.
Key Contributors
· Emily Cantrell, MD | Division of Acute Care Surgery, Faculty | Principle Author
Last Updated
July, 2023
References
- Stassen NA, Bhullar I, Cheng JD, et. al. Selective nonoperative management of blunt splenic injury: An Eastern Association for the Surgery of Trauma practice management guidelines. J Trauma Acute Care Surg. 2012;73(5): S294-300.
- Rowell SE, Biffl WL, Brasel K, et. al. Western Trauma Association critical decisions in trauma: Management of adult blunt splenic trauma—2016 updates. J Trauma Acute Care Surg. 2016; 82(4): 787-93.
- Wallen TE, Clark K, Baucom MR, et al. Delayed splenic pseudoaneurysm identification with surveillance imaging. J Trauma Acute Care Surg. 2022;93(1):113-117.
- Freeman JJ, Yorkgitis BK, Haines K, et al. Vaccination after spleen embolization: A practice management guideline from the Eastern Association for the Surgery of Trauma. Injury. 2022;53(11):3569-3574.
